
Improving Documentation Quality and Creating Time for Core Activities |
Success factors for implementing AI-based documentation systems in nursing care
| Journal | Industry 4.0 Science |
| Issue | Volume 42, 2026, Edition 1, Pages 154-160 |
| Open Access | https://doi.org/10.30844/I4SE.26.1.146 |
| Bibliography | Share | Cite | Download |
Abstract
Keywords
Article
AI-supported nursing documentation: expectations and reality
Artificial intelligence (AI) refers to the capability of computer systems to perform tasks that typically require human intelligence, such as language processing, decision-making, or pattern recognition [1]. The use of AI systems in nursing care is widely considered as a promising approach to increasing efficiency, improving care quality, and reducing workload pressure for nursing staff [2]. In particular, administrative tasks such as billing and documentation offer substantial potential for AI-based support [3–6].
Systems incorporating speech recognition or real-time data processing can accelerate documentation processes, reduce sources of errors, and enable more accurate assessment of care needs through automated analysis of digital data. In addition, AI systems allow for the analysis of large data sets to identify patterns, anticipate care needs, and detect potential risks at an early stage. This provides a foundation for more individualized care planning and creates temporal resources for direct care and interpersonal interactions. In this way, care quality may be enhanced while contributing to sustainable workload relief for nursing professionals [7].
However, nursing practice indicates that AI-based systems have not yet been implemented on a broad scale and that their potential remains only partially realized [8]. Barriers include ethical and data protection concerns [9], as well as the need to establish appropriate technical, financial, organizational, and personnel conditions for successful and sustainable implementation. Overcoming these barriers requires deliberate and context-sensitive organizational efforts rather than peripheral adoption [10].
Human-centered introduction of AI-based documentation systems in nursing care
From a socio-technical perspective, the introduction of digital technologies does not automatically lead to improvements or deteriorations in efficiency and work quality [10]. Sustainable improvements in terms of ‘joint optimization’ require a close alignment between technological innovations and the needs, capabilities, and everyday work realities of users. In addition, organizational structures, technical requirements, and external influencing factors, such as the needs of care recipients, must be considered.
For AI-based documentation systems, this implies that their introduction must be closely aligned with existing nursing processes and institutional frameworks. In order to create added value, the design and implementation of these systems should follow a human-centered approach. This means that systems should be designed to consider the needs and requirements of the people who use them or are affected by them, with the aim of promoting efficiency, satisfaction, and well-being [11]. Nursing professionals, as primary users, must be able to perceive the technology as a form of support in their daily work.
Accordingly, successful and sustainable implementation requires a context-sensitive and participatory approach that involves all relevant actors in the care process [12]. This requirement is not limited to the introduction and use of AI but applies to technological innovations in work and organizations more broadly. However, given the comparatively low level of digitization in nursing care, AI implementations as ‘joint optimization’ processes are likely to be particularly demanding in this context and to entail increased requirements, especially with regard to acceptance and qualification [3, 4].
Objective and methodological approach
While current research on AI in nursing care often focuses on generating nursing diagnoses or care plans based on existing electronic patient data [13, 14], this contribution shifts the focus to the preceding process of data collection, extraction, and documentation. Specifically, the study examines AI-supported documentation systems based on speech-to-text models that capture, structure, and classify relevant information from admission interviews in real time.
Admission interviews are conducted as part of the Structured Information Collection (SIS), a core component of nursing process planning [15]. The SIS serves the systematic collection of care relevant information across six thematic domains (cognitive and communicative abilities, mobility and agility, disease-related requirements and stresses, self-care, social relationships, behavioral patterns and psychological problems) and thus provides the basis for nursing assessment, risk evaluation, and care planning [15].
The SIS is conducted as an open conversation at the beginning of the care relationship and requires considerable time and personnel resources, particularly when documentation is performed in analog form and subsequently digitized. At the same time, high documentation quality is essential, as it forms the foundation for appropriately tailored care services.
The use of speech-processing AI systems aims to support this process simplifying documentation and automatically extracting relevant information and assigning it to SIS categories, thereby reducing workload of nursing staff.
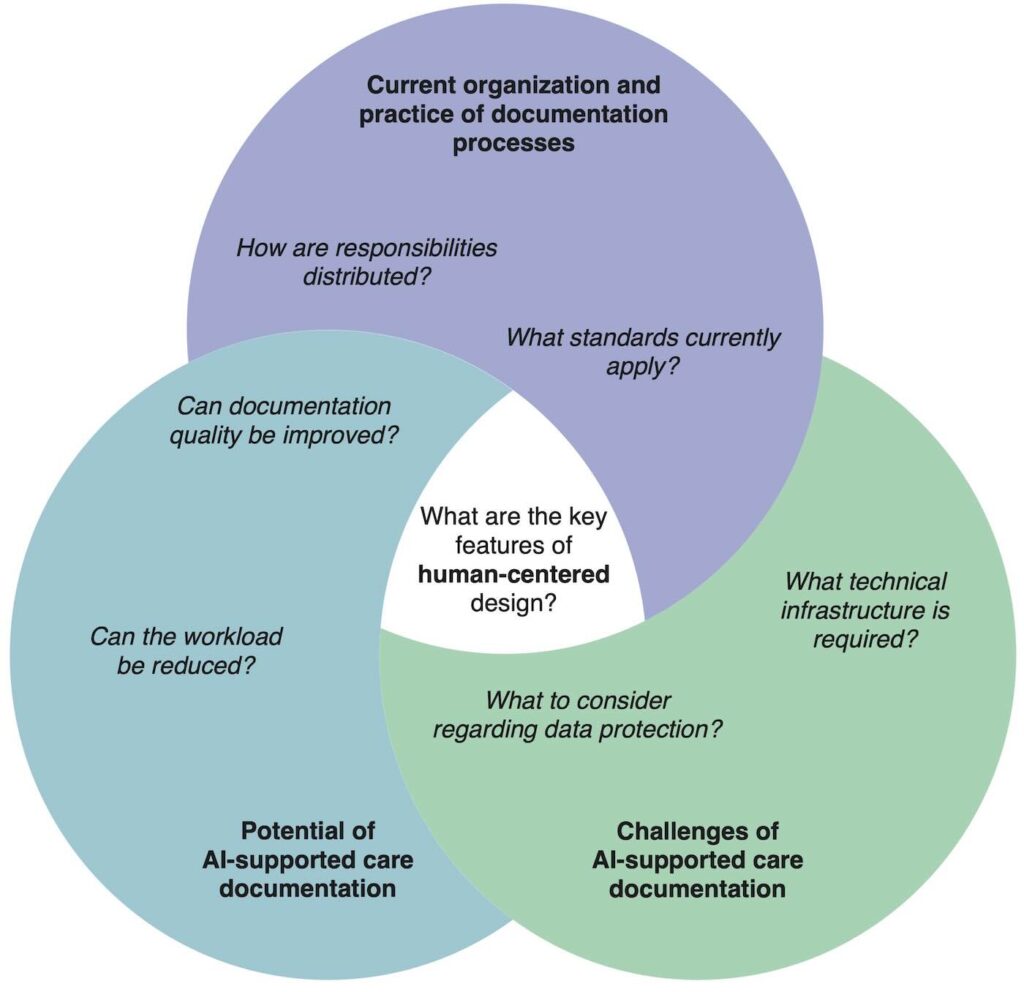
The objective of this contribution is to examine to what extent such systems can actually contribute to improvements in work quality and quality of care, and which conditions must be met for their sustainable and successful implementation and use. Specifically, the study addresses the following research question: What requirements and implications arise for the design of work with AI systems in nursing care that promote ethically desirable objectives in terms of decent work (Figure 1).
To address this question, a total of 19 qualitative semi-structured interviews were conducted between October 2022 and July 2023 with nursing professionals (7) and nursing experts (12), including nursing managers and quality management representatives, across outpatient and inpatient care facilities of varying size (approx. 80 to 800 employees). The sample allowed for a multi-perspectival view that integrates both the experiences of nursing staff and the perspectives of those responsible for the introduction and design of technical systems.
Data analysis followed an inductive approach using structured content analysis [16]. The interview material was initially coded by two researchers using the main categories of challenges, potential, and design requirements, which were subsequently refined into subcategories for further differentiation. Discrepancies were discussed within the author team and resolved by consensus.
Challenges of existing documentation processes in nursing practice
The interviews with nursing professionals and nursing experts reveal a fragmented approach to the collection and subsequent processing of information from admission interviews. Documentation responsibilities are often distributed across multiple actors and vary widely regarding available time resources and organizational procedures. In addition, participants report heterogenous forms of preliminary documentation, including handwritten notes, memory-based records, and digital memos, which then serve as the basis for formal digital documentation.
A central challenge concerns the lack of clearly defined responsibilities, resulting in delayed or incomplete documentation. This, in turn, can lead to situations in which a comprehensive overview of care is not available during ongoing care provision:
“[…] we sometimes have clients who receive wound care for six weeks and the SIS is still not completed until they leave the care service.” (Facility B, Interv. 9, nursing professional)
According to four of the seven interviewed nursing professionals, insufficient standardization and SIS criteria that are perceived as difficult to understand contribute to uncertainty in nursing documentation practices. In addition, five nursing professionals emphasize inadequate time resources for conducting admission interviews and the associated documentation. Overall, documentation conditions are predominantly experienced as burdensome, both due to the substantial time required and because they restrict what is perceived as the “actual” nursing work, namely the direct care and support of care recipients.
Potentials of AI-supported nursing documentation from the perspective of nursing practice
The use of digital and in particular AI-based documentation systems is associated with expectations of reduced documentation workload and improvements in both work quality and quality of care. The interviews indicate that some facilities are already using forms of digital support, such as applications that allow care-related information about care recipients to be assessed and documented. In one facility, speech recognition software is additionally used to record information directly on mobile devices, thereby reducing information loss.
The majority of nursing professionals primarily emphasize the potential for time savings, accompanied by the expectation of gaining more time for direct care and interaction. Furthermore, it is expected that systems capable of automatically filtering, assigning, and standardizing conversational content may reduce inaccuracies in documentation and compensate for uncertainties, for example those arising from language barriers or difficulties in navigating the SIS structure.
“[…] Nursing professionals are practitioners rather than theorists, and already with the introduction of SIS it became clear that more consistent training would have been needed […] on what exactly has to be done. If there was a system behind it that knew how information should be assigned and which aspects are important, […] in which categories, this would reduce the error rate.” (Facility B, Interv. 9, nursing professional)
Additionally, nursing experts highlight the potential of AI-supported data processing to improve interface communication and the further utilization of relevant information. For example, systems could generate early indications of care needs or risk constellations:
“For example, alarm signals […] where certain combination of […] risk factors increase the likelihood of falls or when it becomes apparent that nutritional problems are emerging […].” (Facility L, Interv. 18, nursing expert)
Across interviews, the overarching goal articulated is to make nursing documentation more efficient and of higher quality. In terms of ‘joint optimization’ this is expected to enhance both work and documentation quality while sustainably improving the care provided to care recipients.
Identified design requirements for AI-supported nursing documentation
For AI-based systems to effectively improve documentation and work quality in nursing care, technical, organizational, and personnel-related conditions must be considered at an early stage and aligned with one another.
Many nursing professionals report uncertainties in documentation work. Training opportunities are perceived as insufficient, as they scarcely address practical application in everyday work, both in analog and digital contexts. More than half of the interviewed nursing professionals anticipate that AI-based systems may initially create additional demands. Without targeted training, there is also a risk of unequal use: while digital confident employees may use new technologies efficiently, the potential remains largely inaccessible to nursing professionals who feel insecure about technology. Both groups therefore emphasize the importance of a structured introduction process accompanied by continuous opportunities for practice and information:
“[…] far too little importance is attached to this […], i.e., the introduction process. Many projects […] fail at this point. Acquiring a technology alone does not yet lead to its actual use.” (Facility G, Interv. 13, nursing expert)
At the same time, existing uncertainties should be taken as an opportunity to clearly define responsibilities and documentation standards. As a further prerequisite, respondents emphasize the need for a reliable digital infrastructure. More than half of the participants report missing Wi-Fi, unstable mobile connections, and insufficient technical equipment:
“I see challenges in the […] internet connection. Often there is none, […] and in rural areas there is frequently no mobile data either. […] That becomes problematic when we cannot access the software […].” (Facility B, Interv. 9, nursing profeessional)
These deficits hinder the integration of AI-based systems and often result in the parallel use of analog and digital documentation, thereby counteracting the intended workload relief.
Finally, concerns related to data protection among care recipients must be also addressed. Older generations in particular often express reservations toward technology-supported procedures, leading nursing experts to anticipate acceptance problems:
“We mainly work with people who did not grow up with technology, […] and these are often individuals who have serious concerns […]. It is very difficult to achieve acceptance for its use.” (Facility I, Interv. 15, nursing expert)
Overall, the successful implementation of AI-based nursing documentation requires not only functional technology, clearly defined responsibilities, and targeted training, but also sensitivity in addressing the concerns of all involved stakeholders.
Summary and outlook
The findings indicate that AI-based documentation systems have the potential to contribute to the optimization of documentation and work processes in nursing care. Nursing professionals and nursing experts express predominantly positive assessments and emphasize the potential for improving both the documentation quality and quality of care. At the same time, the results make clear that more efficient processes and temporal workload relief do not emerge automatically. Rather, attention to critical success factors is essential for the sustainable and human-centered implementation of such systems (Figure 2).
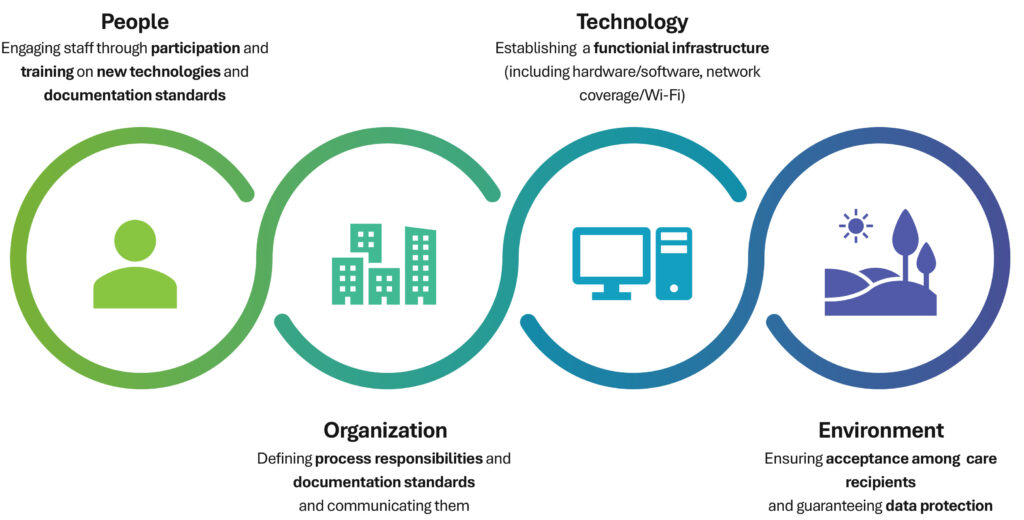
A key requirement is to consider system usability as well as the technical, organizational, and personnel-related conditions of implementation. The needs and expectations, as well as the concerns of nursing professionals and care recipients should be identified at an early stage, with participatory design approaches developed and closely aligned with existing work processes. Opportunities for practical testing and targeted qualification measures, such as micro-training sessions conducted directly at the workplace, support the safe and confident use of new systems.
In this context, the concept of employee dialogue [17], a participatory workshop and dialogue format designed to systematically involve employees in the development and introduction of AI solutions, may serve as a useful instrument for unlocking potential improvements in both care and work quality.
Overall, the findings and derived implementation requirements contribute to the promotion of human-centered work design while simultaneously addressing central ethical objectives, including decent work and participation. In doing so, this contribution integrates a work design perspective with an ethical normative lens on the introduction of AI-based systems in nursing care.
This article was written as part of the HUMAINE research project, which was funded by the BMFTR funding program “Zukunft der Wertschöpfung – Forschung zu Produktion, Dienstleistungen und Arbeit” (funding code: 02L19C200). We would like to thank Alexander Bendel and Maike Wefringhaus for their support in preparing and conducting the interviews.
Bibliography
[1] Kaplan, A.; Haenlein, M.: Siri, Siri, in my hand: Who’s the fairest in the land? On the interpretations, illustrations, and implications of artificial intelligence. In: Business Horizon 62 (2019) 1, pp. 15-25.[2] Peters, M.: KI in der ambulanten Pflege: Fantasie oder Unterstützung? In: Pflegewissenschaft 77 (2024) 4, pp. 52–55.
[3] Seibert, K.; Domhoff, D.; Bruch, D.; Schulte-Althoff; Fürstenau, D.; Biessemann, Felix; Wolf-Ostermann, K.: Application Scenarios for Artificial Intelligence in Nursing Care: Rapid Review. In: Journal of medical internet research 23 (2021) 11. DOI: 10.2196/26522.
[4] Braeseke, G.; Pflug, C.; Tisch, T.; Wentz, L.; Pörschmann-Schreiber, U.; Kulas, H.: Umfrage zum Technikeinsatz in Pflegeeinrichtungen (UTiP). Sachbericht für das Bundesministerium für Gesundheit (2020). URL: https://www.bundesgesundheitsministerium.de/fileadmin/Dateien/5_Publikationen/Pflege/Berichte/2020-06-26_IGES_UTiP_Sachbericht.pdf, accessed 25.05.2025.
[5] Mandl, H.: Die Digitalisierung verändert (auch) die Pflege. Robotik, Sensorik und KI im Berufsalltag. In: PRO CARE (2022) 3, pp. 40–42.
[6] Lutze, M.; Trauzettel, F.; Busch-Heinzmann, A.; Bovenschulte, M.: Potenziale einer Pflege 4.0: Wie innovative Technologien Entlastungen schaffen und die Arbeitszufriedenheit von Pflegefachpersonen in der Langzeitpflege verändern. Gütersloh 2021. DOI: 10.11586/2021037.
[7] Irmler, M.: Künstliche Intelligenz in der Pflege. In: HEILBERUFE (2023) 75 (44-46).
[8] Schmidt, L.: KI in der Langzeitpflege: Potenziale bisher kaum genutzt. In: PFLEGE Zeitschrift 77 (2024) 4, pp. 24–26.
[9] Schüz, B.; Urban, M.: Unerwünschte Effekte digitaler Gesundheitstechnologien: Eine Public-Health-Perspektive. In: Bundesgesundheitsblatt 63 (2020), pp. 192–198.
[10] Parker, S. K.; Grote, G.: Automation, Algorithms, and Beyond: Why Work Design Matters More than Ever in a digital world. In: Applied Psychology, 71 (2022) 4, pp. 1169–1653.
[11] ISO 9241-210:2019. Ergonomics of human-system interaction (2019).
[12] Winby, S.; Mohrman, S. A.: Digital Sociotechnical System Design. In: The Journal of Applied Behavioral Science 54 (2018) 4, pp. 399–423.
[13] Ju, H.; Park, M.; Jeong, H.; Lee, Y.; Kim, H.; Seong, M.; Lee, D.: Generative AI-Based Nursing Diagnosis and Documentation Recommendation Using Virtual Patient Electronic Nursing Record Data. In: Healthcare Informatics Research, 31 (2025) 2, pp. 156–165. DOI: https://doi.org/10.4258/hir.2025.31.2.156.
[14] Johnson, L. G.; Madandola, O. O.; Dos Santos, F. C.; Priola, K. J. B.; Yao, Y.; Macieira, T. G. R.; Keenan, G. M.: Creating perinatal nursing care plans using ChatGPT: A pathway to improve nursing care plans and reduce documentation burden. In: The Journal of Perinatal & Neonatal Nursing, 39 (2025) 1, pp. 10–19. DOI: https://doi.org/10.1097/JPN.0000000000000831.
[15] Becker, W.: Prozess der Pflegedokumentation und Auswirkungen der Digitalisierung. In: Kubek, V.; Velten, S.; Eierdanz, F.; Blaudszun-Lahm, A. (Hrsg): Digitalisierung in der Pflege. Berlin/Heidelberg 2020, pp. 119–130.
[16] Kuckartz, U.: Qualitative Inhaltsanalyse. Methoden, Praxis, Computerunterstützung, 4. Ausgabe. Weinheim/Basel 2018.
[17] Gerlmaier, A.; Bendel, A.: Wie kollegial ist Künstliche Intelligenz? Risikowahrnehmungen und Gestaltungsanforderungen aus Sicht von Beschäftigten. IAQ-Report 2024-01. Duisburg 2024.





